There are hundreds of top health insurance plans available from the nation’s biggest companies. But which policy is best for you? And how much does it cost? Naturally, the answers are complex, since they depend on your individual needs, personal budget, and how much risk you are willing to take. Another important factor is the cost and availability of an employer-provided policy, and how much of the premium will be paid by your workplace plan.
Your work coverage may be very basic with a high deductible placed on all claims. Or, it may be a “Cadillac” type plan where you have very few, or no out-of-pocket costs. Of course, those types of options are rarely offered any more, especially from smaller companies. And many large and small corporations are no longer offering “no-deductible” healthcare benefits, since it is cheaper to pay an Obamacare tax. The money saved can be used to increase employee job security.
Employers with 50 or more full-time employees must offer “affordable” healthcare benefits to their workers. Dependents under age 26 must also be offered coverage. If 95% of full-time employees are not offered benefits, the penalty could be $2,320 per employee (the first 30 employees are excluded). If the coverage is determined to be “not affordable, the penalty could be as much as $3,840 per employee that purchased a subsidized Marketplace plan. A “full-time” employee is defined as someone who works at least 30 hours per week.
Group Medical Insurance
Group medical insurance (also referred to as “employer-sponsored) is available from most large and small companies. Typically, the larger the size of the company, the bigger the contribution by that employer towards its employee healthcare costs. Often, group health insurance rates much are more expensive (because of lower deductibles on major claims) than personal health care coverage.
Thus, if the employer is not paying a large portion of the premium, purchasing coverage yourself may be an option to consider. And if you are near an “open enrollment” period, it’s always a good idea to verify that no major changes are coming, especially if benefits are going to be eliminated.
However, it’s critical to understand that if offered “affordable” coverage by your employer (less than 8% of your household income), you are not eligible for a federal subsidy. This assumes that the group policy includes 10 required “essential health benefits.” The 8% calculation is based on the cost of the primary employee’s cost of coverage, and not the entire family. Thus, if the employer is paying the cost of the primary worker’s plan, but not the spouse or dependents, it may be difficult to qualify for financial assistance.
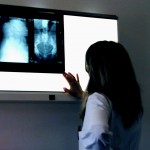
The Best Medical Plans Can Be Yours!
When filling out an application for an individual health plan, it’s important to consider the rate, coverage, and what out-of-pocket expenses are likely to occur. When applying for coverage, if you are being treated for an existing condition, although your rate is not impacted, the likelihood of reaching a lower deductible may be higher. The final determination will be provided in writing, and before accepting the offer, a comprehensive comparison should be made between the personal and group plans.
Usually, when you are accepted, you have a window (perhaps 10-60 days) that allows you to study and compare your new policy and decide if you wish to keep it. But if you wait too long, you may miss the Open Enrollment deadline. And there’s always a chance that the premium will have increased.
Obamacare (Patent Protection And Affordable Care Act)
It is important to understand the impact of recent legislation on how you apply for the top health insurance plans, and how much you pay. Underwriting (starting in 2014) is solely based on where you live, your age, whether you smoke, and how much money you make. Thus, whether you are in impeccable health or on “your death bed,” it won’t make a difference. Also, if your income is below 400% of the Federal Poverty Level, you qualify for a federal tax subsidy.
Since it is quite possible that your rate will increase more than 10% annually, it may be necessary to change to a different plan almost every year. Since there is no termination penalty, and Open Enrollment allows you to freely change policies, we highly endorse the idea of comparing all options before you renew an existing policy. However if your household income has changed, your new subsidy amount may impact the type of policy you choose.
Limited Benefit Insurance
Limited benefit plans provide somewhat affordable medical options to persons with multiple or major health conditions. Often, the plans offer very basic office visit and prescription coverage and extremely high out of pocket expenses on hospital stays. They should only be used with caution and of course, the “fine print” should always be read at least twice! If you’re not sure if you have this type of plan or are being quoted this type of contract, simply ask us. Several companies offer a few limited benefit options that may be appropriate in some circumstances.
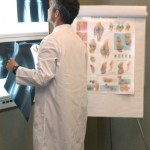
Obamacare Means No Medical Questions!
Limited benefit policies tend to have very high turnover rates and often charge you an application fee, which is another reason we don’t actively market the product. The application fee is sometimes loosely described and not available for a refund. But the major concern is that these plans are not designed to pay large medical claims, just a portion of them.
They are also “non-compliant” and should never be utilized to replace qualified coverage during an Open Enrollment period. If you are eligible for an SEP exception, Marketplace options should be reviewed first, before considering non-compliant contracts.
But if you can’t qualify for other benefits, this may be your best choice. Perhaps most importantly, most of these plans are NOT Affordable Care Act-compliant and do not contain the 10 “Essential Health Benefits” that are required for policies offered on State Marketplaces.
Medical Discount Plans And Cards
Medical “discount plans” are readily available online and are not considered to be “credible coverage.” Often, the coverage descriptions are vague and large applications are required to activate coverage. Although they are “guarantee issue” policies, we strongly advise against their purchase, since it is likely you’ll pay a large amount of money if you have a catastrophic claim. You might even pay quite a bit for a smaller claim! That’s why it is always important to have an experienced broker review the contract with you.
Overview
Providing unbiased assistance is our specialty and we’ll be happy to help you choose which policy best matches your needs. When you “request a quote” from our website, you’ll be able to easily compare the options that work best for you. That’s the purpose of our website…to be consumer-friendly and offer health care plans at the lowest available rates.
We’ll find the plan that’s best for you, not the insurer. And I know we have said before, but it’s important…You never pay any fees by using our website! When shopping for Exchange/Marketplace coverage in your state, it’s important that you receive a federal subsidy (if you qualify). Since it’s now the law that you must be insured, obtaining the lowest cost is more important than ever before.

